Causes and Consequences of Disturbed Cervical Afferents
Learn how the cervical spine functions as a sensory system. Learn how disturbed cervical afferents affect neck proprioception, balance, vision, and rehabilitation in patients with neck pain, whiplash, and concussion.
Written by
Dr. Hilmar Leonardsson
Medical Lead @ NeckCare
What’s truly fascinating about the cervical spine is its function as a sensory system. The soft tissues of the cervical spine contain a substantial amount of small sensory organs known as mechanoreceptors. Most of these mechanoreceptors are muscle spindles that are located within muscle tissue. The cervical muscles are unique in this regard, particularly the suboccipital muscles, which contain the highest muscle spindle density of all the muscles in the body. The role of these mechanoreceptors is to detect mechanical changes within tissue and give us the ability to sense the position and movement of our head and neck. This ability is usually referred to as proprioception.
Proprioceptive information from the cervical spine is sent from the mechanoreceptors to the central nervous system through neural pathways known as the cervical afferents. Additionally, the cervical afferents have unique connections to the visual and vestibular systems.
It is therefore crucial for clinicians managing neck injuries and neck disorders to be familiar with the role of the cervical spine in the sensorimotor system. In these patients, the function of the cervical mechanoreceptors is often impaired, leading to sensorimotor dysfunction, a missing link that is often overlooked in cervical rehabilitation.
The Cervical Afferents and Their Unique Connections
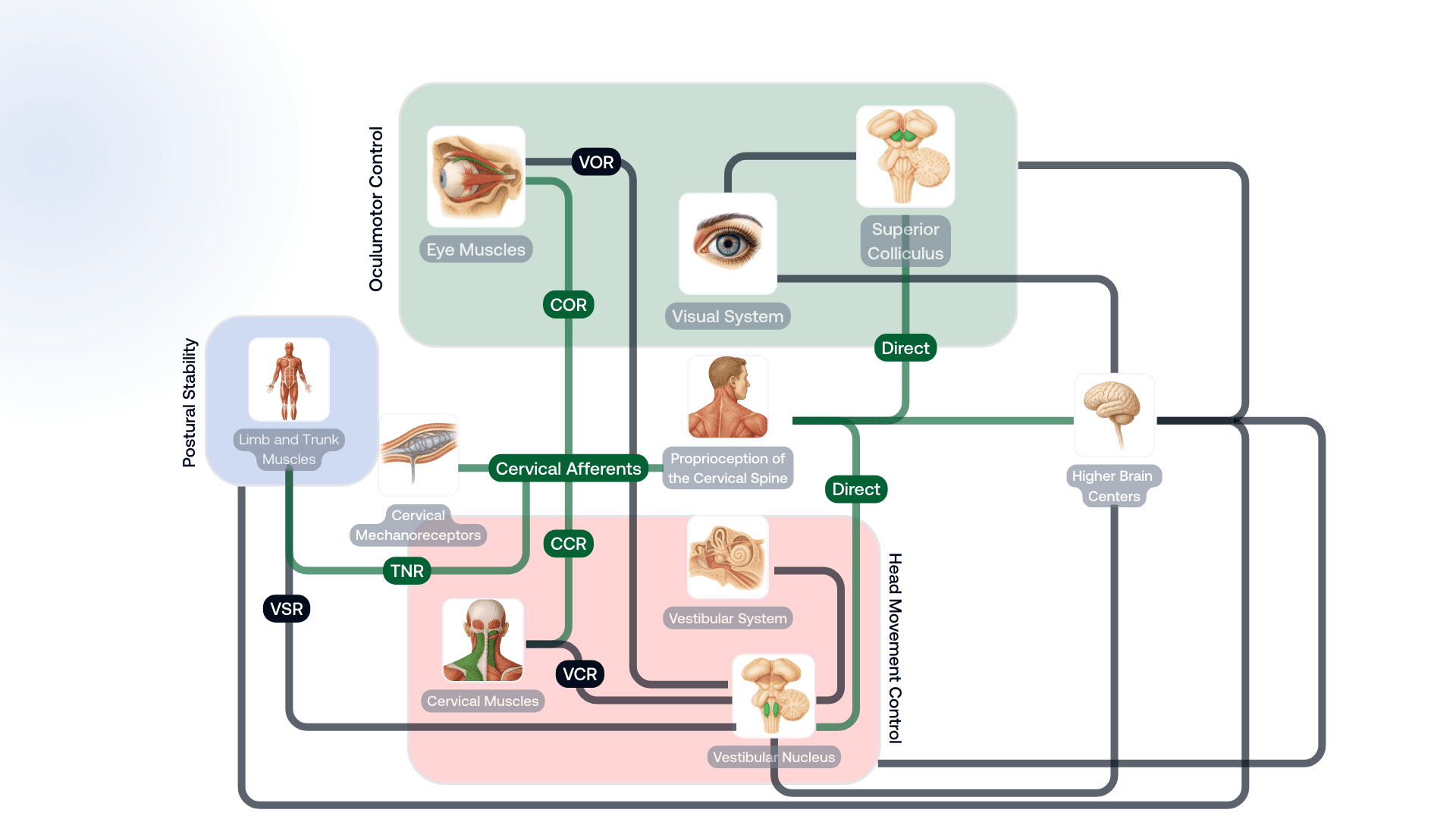
The cervical afferents, the visual and vestibular systems, all send information to higher brain centers for sensorimotor integration. These are structures such as the thalamus, cerebellum, and somatosensory cortex. The three sensory systems are also interconnected through complex reflex pathways and direct neural connections. This integration of cervical proprioception with visual and vestibular input is essential for sensorimotor control, supporting accurate head movement control, oculomotor control, and maintaining postural stability.
The cervical afferents are involved in three main reflex pathways: the cervico-collic reflex (CCR), the tonic neck reflex (TNR), and the cervico-ocular reflex (COR). The CCR works together with the vestibulo-collic reflex (VCR) to activate neck muscles and control head movements. The TNR integrates with the vestibulo-spinal reflex (VSR) to activate limb and trunk muscles, helping to maintain postural stability. Finally, the COR integrates with the vestibulo-ocular reflex, activating extraocular muscles to control eye movements. Beyond these reflexes, the cervical afferents also have direct neural pathways to the vestibular nucleus and the superior colliculus, a coordination center for eye and head movements, which means that proprioceptive input from the cervical spine is used to shape the output of these visual and vestibular structures.
This allows cervical proprioceptive input to quickly influence the visual and vestibular systems without first requiring processing in higher brain centers. The cervical spine is likely the only musculoskeletal region in the body that has this direct access to the visual and vestibular systems. This helps explain why injuries and pain in the cervical spine often lead to sensorimotor dysfunction, which can cause a wide variety of symptoms not typically seen in injuries to other musculoskeletal regions of the body.
Disturbed Cervical Afferent Input
Neck pain, cervical spine injuries, and other neck disorders can disrupt the proprioceptive signals sent by the cervical afferents and often lead to sensorimotor dysfunction. This disruption can happen through several different mechanisms, either at the level of the mechanoreceptors or at higher processing levels.
Direct damage
Direct trauma to the cervical mechanoreceptors is a common cause of disrupted cervical afferent input. Local inflammation or ischemia can also induce chemical changes that affect muscle spindle sensitivity. Furthermore, repetitive joint loading can lead to soft tissue laxity, desensitize mechanoreceptors, and impair reflex pathways.
Functional impairment
Altered function of the cervical muscles can also affect mechanoreceptor activity, for instance, increased fatigability or abnormal increase or decrease in muscle tone. It’s also well documented that neck injuries often cause inhibition of deep cervical muscles while superficial muscles are activated simultaneously, and the deep cervical muscles happen to have the highest muscle spindle density.
Pain
Pain itself can also interfere with proprioceptive input on many levels. Peripherally, it can inhibit muscle activity and reduce the sensitivity of muscle spindles. Centrally, it can also modulate proprioceptive input at the spinal cord and higher brain centers, affecting the ability to interpret and integrate proprioceptive information. There is also evidence that psychological stress, through the activation of the sympathetic nervous system, can affect muscle spindle activity.
Structural changes
In chronic neck pain and prolonged cervical dysfunction, structural changes often occur in the cervical muscles. These include transformation from slow to fast-twitch muscle fibers, muscle atrophy, and fatty infiltrations. These structural changes can further compromise mechanoreceptor function, interfering even more with cervical proprioceptive input.
Signs and Symptoms
Since the cervical afferents are integrated with the visual and vestibular systems to control motor outputs, it should be clear that dysfunctions in the cervical spine that disrupt sensorimotor control can lead to symptoms in any of these three sensory systems. These patients often have a history of neck pain, whiplash-associated disorders (WAD), or concussion. Patients may report:
Dizziness, light-headedness, or unsteadiness
Cervicogenic headaches and neck stiffness
Visual fatigue, light sensitivity, or difficulty concentrating while reading
Weak cervical muscles or muscle fatigue
In these patients, it’s important to assess proprioception of the cervical spine, as well as to evaluate if proprioceptive input from the cervical afferents is affecting the patient’s balance, oculomotor control, and coordination. On physical examination, patients with neck pain, WAD, concussion, and other cervical disorders often have deficits in one or more of these components.
Cervical Proprioception
Cervical proprioception is the ability to sense the position, movement, and force of the neck without visual input. If the cervical mechanoreceptors are compromised, this sense can become disrupted. There are two main components of proprioception that are most often assessed in clinical practice, they are joint position sense and movement sense. Joint position sense refers specifically to the ability to perceive the static position of a joint and is usually objectively measured with the joint position error (JPE) test. Movement sense, on the other hand, refers specifically to the ability to detect joint or limb movement, including the direction, speed, and amplitude of motion, and can be objectively measured with NeckCare’s Butterfly test. Patients with neck pain, WAD, or concussion generally perform worse on these tests compared to healthy asymptomatic individuals.
Balance
The cervical afferents can affect balance through the TNR or the vestibular nucleus. Balance needs to be assessed with the neck both in a neutral position and a torsioned position. If the patient demonstrates worse balance with the neck in a torsioned position compared to a neutral position, it may indicate that the cervical afferents are contributing to the balance disturbance. There are also dynamic balance tests that can have clinical value. For example, assessing the patient's balance while walking and simultaneously performing head turns.
Oculomotor control
Disrupted cervical afferent input can affect eye movements through the COR or the superior colliculus. It’s important to bias the cervical component during oculomotor examination, as it can help determine whether proprioceptive input from the cervical spine is affecting eye movements. Gaze stability is often impaired in these patients, meaning they have difficulty keeping their eyes focused on a fixed target while actively moving their head. The smooth pursuit neck torsion (SPNT) test is a clinical test designed to specifically distinguish eye movement disturbances caused by changes in cervical afferent input. In the test, patients have to smoothly track moving objects with their eyes while keeping their head still. Patients with disrupted cervical afferent input tend to perform worse with their neck in a torsioned position compared to a neutral position.
Coordination
When the cervical afferents are transmitting impaired proprioceptive signals, it can affect coordination between eye and head movements. Patients with neck pain and whiplash injuries are known to have both decreased velocity and compensatory head movements when they are performing eye-head coordination tasks. Similarly, the coordination between trunk and head movements can be impaired, where patients often struggle to keep their heads steady while actively moving the trunk.
By systematically evaluating these components, the clinician can gain a valuable understanding of how the patient's cervical spine is affecting sensorimotor control function. Each sensorimotor test seems to assess a different sensorimotor skill, and there doesn't appear to be a direct relationship between the outcomes of these tests. This means that patients can easily present with an impairment in one of these sensorimotor components, but not in the others. It’s therefore recommended to assess every aspect of sensorimotor function discussed above.
Clinical Management
Evidence indicates that effective management of disturbed cervical proprioception and sensorimotor control should address both any primary musculoskeletal dysfunction and the accompanying sensorimotor control impairments.
When addressing the musculoskeletal component, the goal is to reduce pain, restore range of motion, and increase strength and endurance in the cervical muscles. Many clinical trials have demonstrated the positive effects of musculoskeletal intervention for these patients. However, musculoskeletal interventions alone may not be sufficient or the most efficient way to address sensorimotor deficits.
Sensorimotor dysfunctions are most effectively treated with rehabilitation programs that specifically target the impaired sensorimotor function. These exercises should be done in short sessions at least once a day, preferably twice, beginning with 3-5 repetitions and gradually increasing to about 10 repetitions per exercise.
Training that targets cervical joint position sense, eye–head coordination, and gaze stability improves not only sensorimotor control but also reduces neck pain, disability, and improves range of motion. Accordingly, current evidence supports that an integrative treatment approach, incorporating both musculoskeletal and sensorimotor interventions, leads to improved outcomes for patients with neck pain, WAD, or concussion.
References
Macefield VG. Physiological characteristics of low-threshold mechanoreceptors in joints, muscle and skin in human subjects. Clin Exp Pharmacol Physiol. 2005;32(1-2):135-144. doi:10.1111/j.1440-1681.2005.04143.x
Kulkarni V, Chandy MJ, Babu KS. Quantitative study of muscle spindles in suboccipital muscles of human foetuses. Neurol India. 2001;49(4):355-359.
Kristjansson E, Treleaven J. Sensorimotor function and dizziness in neck pain: implications for assessment and management. J Orthop Sports Phys Ther. 2009;39(5):364-377. doi:10.2519/jospt.2009.2834
Treleaven J. Sensorimotor disturbances in neck disorders affecting postural stability, head and eye movement control. Man Ther. 2008;13(1):2-11. doi:10.1016/j.math.2007.06.003
Peng B, Yang L, Li Y, Liu T, Liu Y. Cervical Proprioception Impairment in Neck Pain-Pathophysiology, Clinical Evaluation, and Management: A Narrative Review. Pain Ther. 2021;10(1):143-164. doi:10.1007/s40122-020-00230-z
Jull G, Falla D, Treleaven J, O’Leary S. Management of Neck Pain Disorders: A Research Informed Approach. 1st ed. Elsevier Churchill Livingstone; 2018.
Treleaven J. Clinical recognition of the role of the cervical spine in signs and symptoms of altered sensorimotor control. Musculoskelet Sci Pract. 2024;74:103187. doi:10.1016/j.msksp.2024.103187
de Zoete RMJ, Osmotherly PG, Rivett DA, Snodgrass SJ. Seven cervical sensorimotor control tests measure different skills in individuals with chronic idiopathic neck pain. Braz J Phys Ther. 2020;24(1):69-78. doi:10.1016/j.bjpt.2018.10.013
Revel M, Minguet M, Gregoy P, Vaillant J, Manuel JL. Changes in cervicocephalic kinesthesia after a proprioceptive rehabilitation program in patients with neck pain: a randomized controlled study. Arch Phys Med Rehabil. 1994;75(8):895-899. doi:10.1016/0003-9993(94)90115-5
Jull G, Falla D, Treleaven J, Hodges P, Vicenzino B. Retraining cervical joint position sense: the effect of two exercise regimes. J Orthop Res. 2007;25(3):404-412. doi:10.1002/jor.20220
Storaci R, Manelli A, Schiavone N, Mangia L, Prigione G, Sangiorgi S. Whiplash injury and oculomotor dysfunctions: clinical-posturographic correlations. Eur Spine J. 2006;15(12):1811-1816. doi:10.1007/s00586-006-0085-0
Published on
Written by
Dr. Hilmar Leonardsson
Medical Lead @ NeckCare